|
Abram and I are finally back from his surgery at the Mayo Clinic where he underwent an airway endoscopy (all the way down to the bronchial tubes) as well as an adenotonsillectomy - where they surgically removed his tonsils and his adenoid. I thought I'd share our experience here because as my son suffered and while I madly googled for ways to alleviate his suffering in the middle of the night - I found zero information about kiddos with special needs having this type of surgery done. So, I am going to share how things went with Abram because healing and surgery for a child with special needs and major sensory issues is vastly different than that of a typical child. For most children, these types of procedures are outpatient and the child gets to return home to recover. For children like Abram who have a history of neurological issues/sensory issues, they recover during a hopefully brief stay in the PICU as well as at least an overnight hospital admission and for us a medically required 14 days away from home and near the ER of Mayo incase anything went wrong. I'm sharing this particular journey because we got a lot of good advice that may or may not work for your situation. For Abram - who is non-verbal, has a seizure history and has major sensory issues/tactile issues and feeding issues - this was NOT an easy task but we got through it. Suggestions for other parents can be found at the bottom. Although all sweet and well-meaning ideas - none of them would work for Abe because he doesn't do cold/wet/squishy, ever. I literally tried everything - food and drink wise to try to make him comfortable but he wanted nothing to do with it and the ENT basically said that Water was the best thing for him, anyhow. I stocked up on Pediasure, Apple Juice, Boost, Almond Milk, Mac n' Cheese, Soft Muffins, etc. He wanted nothing to do with any of it. My Summary: Abram would not eat at first, period. We were repeatedly reassured that this was "normal". His breath literally smelled like a carcass that would most likely gag a vulture. He sounded raspy when he slept and he needed around-the-clock medication alternating Tylenol and Ibuprofen every 3 hours, no matter what. Set your alarms and don't miss a dose, period. If your child is old enough and can tolerate suppositories, do it. Abram did NOT want to swallow and we had to restrain and force medicine (as instructed by the nurse) but for his age/weight there were no suppositories for us to use and I am not certain that would have gone over well, either. The only thing that helped us keep him somewhat behind the pain was the ability to dose his cannabis oil - and that is clearly not even an option for everyone. Water was KEY. We used a tiny plastic dixie cup and made him drink that every 30 minutes. They NEED 3-4 wet diapers a day. Abram was having 2-3 and it was making the nurses nervous and we were nearly on the verge of having to go back for IV fluids but thankfully pushed through it. He seemed to enjoy his baths and would actually drink the warm bath water willingly. Day 1 - March 10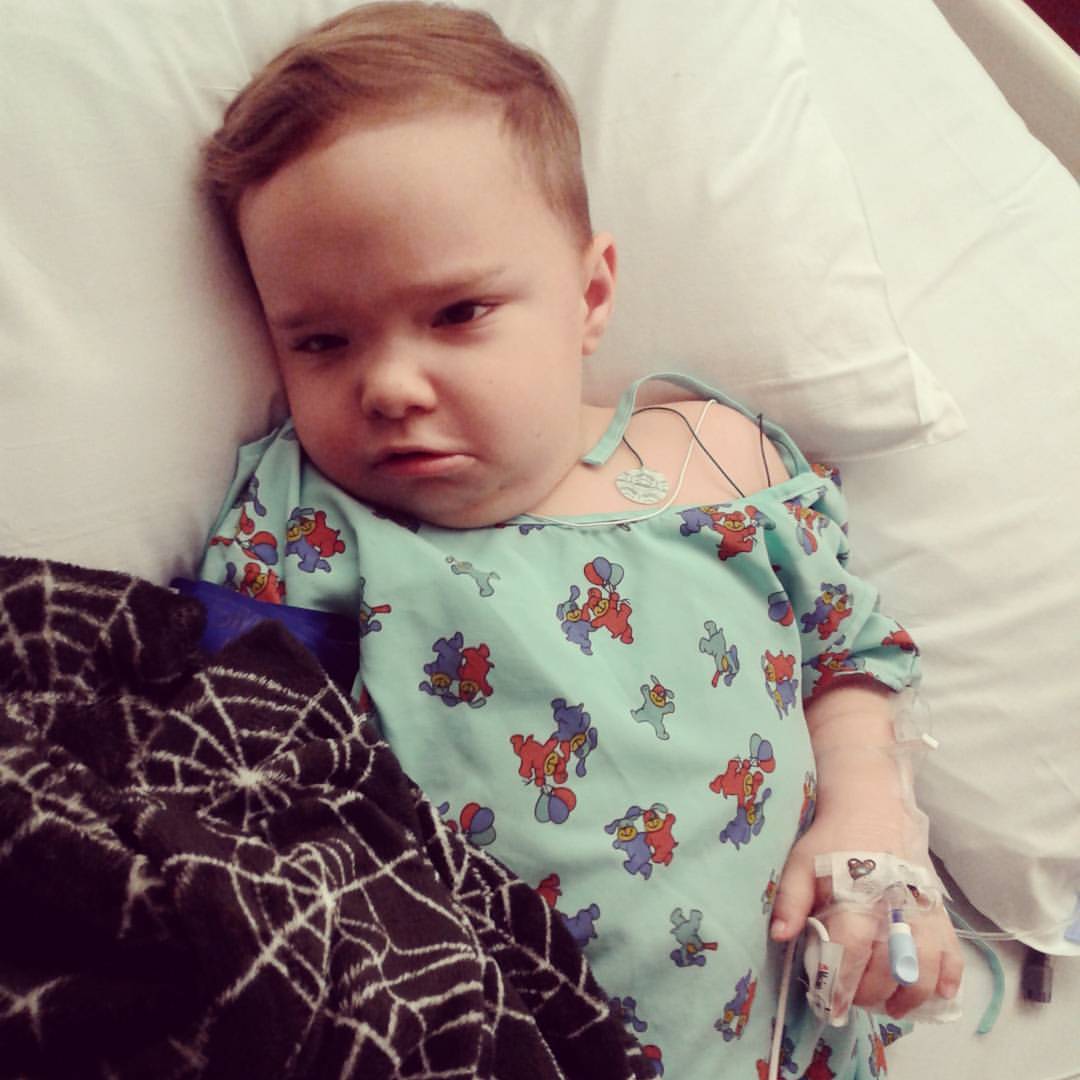
Abram was scheduled to arrive at the Hospital (St. Mary's) by 8:30 am on a Friday. We arrived on-time and had withheld food and drink as required for the surgery. Our surgery actually ended up being pushed back 5 hours because there was an emergency/accident that came into the Hospital that required our surgeon.
Abram was being a good boy (and actually napped) but by the time we got to the pre-op room, he was getting agitated as he'd been without food or drink for 17 hours and did not understand what was happening. Mayo is great about sending in Child Life people to try to find toys to entertain your child. Abram was appeased by a weird long vibrating tube that he chewed on while we spoke with the Anesthesiologist. They gave Abram a dose of Versed to help relax him before he had to go to the Operating Room, which is used to help calm kids/make them sleepy. However, it is also a benzodiazepine - which we just spent 18+ months weaning out of our son's body because another benzo (Klonopin) caused more frequent and worsening seizures. Of course, as soon as the Versed kicked in, the anesthesiologist extensively warned us about how all of this just may indeed trigger a seizure and that IF he were to have one, to realize it was from all the medicine and the anesthesia and would not necessarily mean that his seizure-free streak was over. This made me scared and Abe was *still* nervous and agitated so after trying to squeeze me into a "one-size-fits-some" surgical outfit they wrapped me up in two different gowns (talk about embarrassing) so that I could actually go into the OR with Abram. Once gowned up, I laid on Abram's bed with him and they actually rolled me back into the Operating Room with Abram so that he could be with me until he fell asleep. Unfortunately, the nurse in the room decided to move him to the operating table before getting the Ok from the Anesthesiologist and tried putting on the 02 monitor on Abram's fingers - which actually woke him up and caused him to be very upset. The anesthesiologist told her to back off and gave her a good bit of advice about how there was a reason I was in there with my child, that he was anxious and that she shouldn't have touched him. I left the room with a smirk on my face but felt good that at least there was someone in that room with my boy who GOT HIM. Abe's Dad and I were told that the surgery would take 2 hours and by now it was 2:00 in the afternoon so we tried to go get lunch with the apology vouchers we were given but the cafeteria was closed so we had to run across the street to go get some food. We were given a pager before we left and we warned to get back as soon as possible if it went off. Within an hour, the pager went off and we ran back to the surgical floor as fast as we could - worried that something had happened - only to find out that he was out of surgery and that the Surgeon wanted to speak with us. She told us that his surgery went well without issues, that she found some "cobblestoning" in his throat probably caused by reflux and that otherwise, everything else looked good - as in there were no other obvious reasons for our son to have obstructive sleep apnea with the tonsils and adenoids gone. We waited another hour and were finally able to go see Abram in the PICU. Abram was still asleep when we got in there but he levels were doing good and they were able to take him off of his oxygen without any de-stats within the first hour - which was good. They were still giving him Fentanyl for pain relief but he slowly woke up and only spent 4 hours in the PICU before we were admitted to the Hospital in his own room. The only issue we ran into that night was an issue with a nervous nurse and our son's cannabis oil - but I'll leave that for another post. In the end, he got his medicine, he NEVER seized and Abram was able to drink water that night, which was a huge relief. Day 2 - March 11
Abe was released from the Hospital by 2:00 the next day but he was in a lot of pain. The Hospital gave us a schedule where we were to be alternating pain medicine (Tylenol and Ibuprofen) every 3 hours, which was a chore. Abram was fighting us on taking the pain medicine and had to be restrained just to get the medicine in his mouth. But, he was actually drinking water and even ate some macaroni and cheese so we called that a win.
He slept a lot as I think he was worn out from the whole ordeal of it all but it was good because at least he wasn't hurting when he was asleep. Day 3 - March 12Abe was in a lot of pain on Day Three. Even though he was getting his pain meds as instructed (I even set alarms on my cell phone so I would wake at night/day to give him his meds on-time and keep ahead of the pain). The worse part was, he was running a bit of a fever and he screamed and cried and fought every time we needed to administer the pain meds - which made it worse for him and made it harder on me. This is where his sensory issues come in to play as he was hurting badly but didn't want to eat/drink anything cold and swallowing the medicine seemed painful for him. The bathtub luckily appeased him and he would at least drink some warm tub water so we spent a lot of time sitting in the tub. We had some folks offer us some suggestions like suppositories for pain meds but we could not find any locally that were for kids under the age of 6. There were kept behing the counter at the pharmacies and could not be purchased off-the-shelf so I couldn't even try that as a solution for Abram. Many folks also mentioned that their child got codeine to deal with the pain but our surgeon told us that children with sleep apnea and children under the age of 6 are no longer given codeine because of several deaths in the last 5 years with this exact surgery. So Abram's only option for pain relief was Tylenol, Ibuprofen and his cannabis oil. My mom came up to help and she was great at encouraging Abram to eat some macaroni and cheese and got him to drink several ounces of water out of small dixie cups. Day 4, 5 & 6 - March 13 - 15
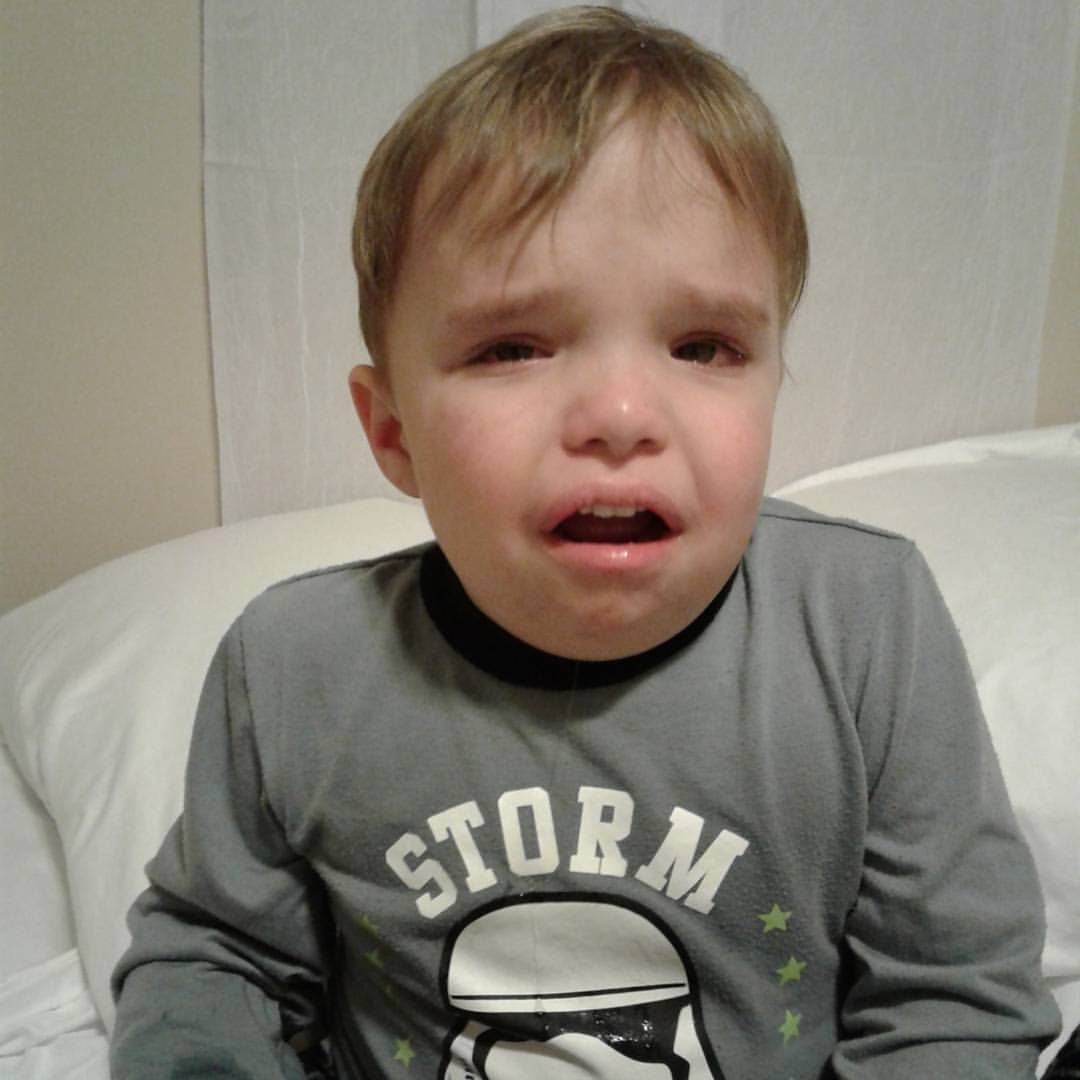
Abram is suffering pretty bad after an airway endoscope down to his lungs and having his tonsils and adenoid removed.
He's been on Tylenol and Ibuprofen every 3 hours plus his cannabis oil and he's still hurting, can't stop whining and hasn't eaten food in about 36 hours. I can still get him to drink tiny amounts of water every 30 mins, so he still has had a few wet diapers but this crap is no joke. He is on the autism spectrum and has major food issues on a good day.. and even then he won't touch cold/frozen foods or anything squishy/wet. Add in pain and he's not interested in eating at all. They say Day 5-7 is when the scabs start sloughing off a little and considering his poor little breath smells like a hot carcass, I'd guess that's another reason he'd have no appetite. I just hate seeing him hurt so badly. Day 7 - March 16
Still hurting. Still hasn't eaten food since Monday except 1/2 a chocolate chip cookie yesterday.
He will drink water little sips at a time. Still has wet diapers. Mom is still worried. I called the Nurse to see if it was okay for him NOT to be eating and they reassured me that it was "normal" but that if he hasn't eaten by noon tomorrow - to call back. Pain management for these little ones seems to be lacking somehow. Update: Abe ate some crackers of all things today around noon. He didn't want anything else the rest of the day but at least he got something else in his tummy besides meds and water. The nurse said his scabs will be coming off soon and judging by his breath, I'd say something foul is going on in there. Poor kiddo.
Day 8 - March 17
Taking a little snooze after being up all night.
We rented a little house up here for the entirety of our stay. So much cheaper than the hotels and so peaceful and quiet. There's a park not far from here that actually has adaptive swings so if/when he feels up to it, we'll try for that again. He keeps signing "Grandma", "kitty" and "swing". I think he misses home. One week down. One to go This day things seemed to be turning around. We were able to get out a bit, go to a park, see some geese and he actually ate some food. But then in the evenings the pain seems to hit harder for some reason and we're right back to worrying. Day 9 - March 18
Still hasn't eaten since yesterday again but he's found a brief reprieve in the tub.
Since Monday he's only eaten a handful of crackers and three nuggets.
Day 10 - March 19
He slept good, ate breakfast and was excited that his Grandpa was coming to visit him.
Day 11 - March 20
Abram's Grandpa came to stay with us for a few days and having him around really brightened his spirits. He finally ate some food, drank some water and was able to play at the park for a bit. But we did notice that he started to suck in his bottom lip, pooling drool that looked like clear slime and was having a hard time swallowing.
Day 12 - March 21
Abram's favorite thing in the world is fire trucks and emergency vehicles so I arranged for a tour at the Fire Station nearest our home to cheer him up! He really liked the 100 year old fire state at Rochester's Fire Station #2 but just as he was getting the chance to sit IN the big firetruck in the garage, an emergency happened and we had to leave in a hurry. He was so upset, he actually bent in half and threw a fit - something I hadn't really see him do. Poor kid. So I scheduled another tour at a larger Fire Station for him before we had to leave.
But by nighttime he was back to hurting pretty bad and was pretty unconsolable and was back to pooling the creepy alien slimey saliva. It was freaking my dad and I out so much that I actually called the on-call Nurse Hotline and after she walked me through several steps on the phone she patched me through to the ER and she was worried that we just needed to go right to the hospital. But once again, we were reassured that all of this was normal and not to worry. It was hard NOT to worry when your kid won't swallow and what is coming from his mouth can be pulled out like strings. Yet, it was clear (smelling of carcass)?! Day 13 - March 22
Abe's a bit chipper again this morning. It seems the key is to keep meds coming every 3 hours. It was chilly but he kept signing "drive, train, you, me, please" so we went to the park and let him hang out in the wooden train that he adored.

The firemen the other day suggested we eat at Mr. Pizza South before we left town.
So, Abe and I ventured over and he had his first experience in an actual pizza parlor and loved it. He of course made friends with the waitress who accepted all his demands while he made me feed him ice water by the straw full. I'm just glad he's feeling better and he ate a slice by himself. Day 14 - March 23
Abe got a tour of Fire Station 1 in Rochester. It was a good pick-me-up for him and we were so thankful to Joe for showing him such a good time and spending some time with us. He had a blast.
Suggestions Made
|
About MeHello! My name is Erin. I am Abram's mom, a tireless advocate for UBE2A Deficiency Syndrome and a fierce proponent for medical cannabis. MOST POPULAR BlOG ENTRYJOIN US
|












 RSS Feed
RSS Feed
